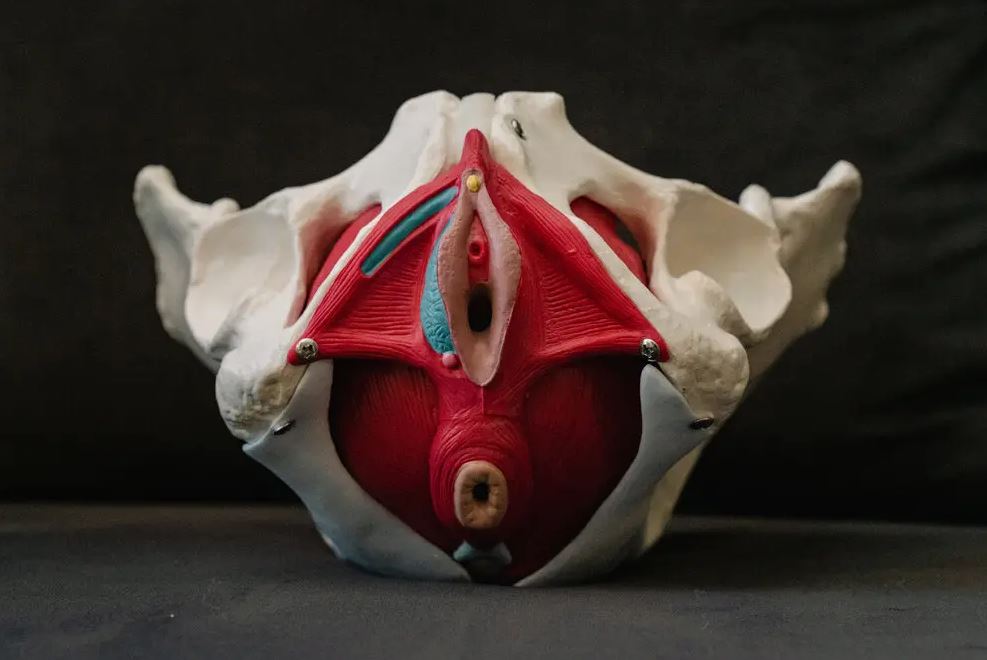
Any medical operation performed on the external genitalia poses a danger to the patient’s ability to have sexual relations. However, other pelvic procedures, such as hysterectomies and surgeries to remove ovarian cysts or endometriosis tissue, may also cause clitoris nerve damage. This is partly due to the fact that the clitoris is so interwoven with the nerve supply in that area.
Even if it makes you uncomfortable, it is important to have an honest conversation with your doctor about your genitalia and sexual orientation before undergoing pelvic surgery. This will help you understand the potential hazards of the procedure and preserve your future sexual sensation. In preparation for your surgery consultation, here are four questions that you should ask.
Are you able to point out the components that will be changed?
Your medical professional need to be able to guide you through the process by showing you diagrams, three-dimensional computer models, or even your own anatomical structure while doing so. You could want to inquire as to the frequency with which the doctor carries out this treatment; ideally, it shouldn’t be the first time he or she does it. Dr. Rachel Rubin, a urologist and sexual health expert based outside of Washington, D.C., recommended that patients “find a new doctor” if their primary care physician seemed evasive or awkward when discussing sensitive health issues.
What are the potential consequences for my sexual experience?
It is essential that you communicate your concerns about arousal, orgasm, and discomfort, as well as your preferences, in as much detail as is feasible. Dr. Rubin posed the following question: “How can your doctor determine whether the potential adverse effects are relevant to you if you never tell them how you feel pleasure?” This may involve inquiring about the potential effects of the treatment on non-genital locations such as the anus, nipples, and cervix.
Do the majority of your patients report experiencing adverse effects?
Be sure that your doctor goes through with you the most frequent adverse effects, all of which should also be noted on the permission form or the post-op statement that you fill out. If your doctor uses a word that you do not understand or that is foreign to you, such as dyspareunia or anorgasmia, ask your doctor to slow down and explain it to you in language that is easier to understand.
Who should I get in touch with if I do end up experiencing long-term sexual negative effects?
Numbness, scarring, problems with arousal, loss of feeling, hypersensitivity, and discomfort that does not improve are some of the side effects that you should be on the lookout for. Dr. Emily Von Bargen, a urogynecologist who works at Massachusetts General Hospital, is quoted as saying, “I normally tell patients, ‘Every day you should feel better.'” If your symptoms do not begin to improve, talk to your primary care physician about getting the names of sexual health professionals that you may contact.