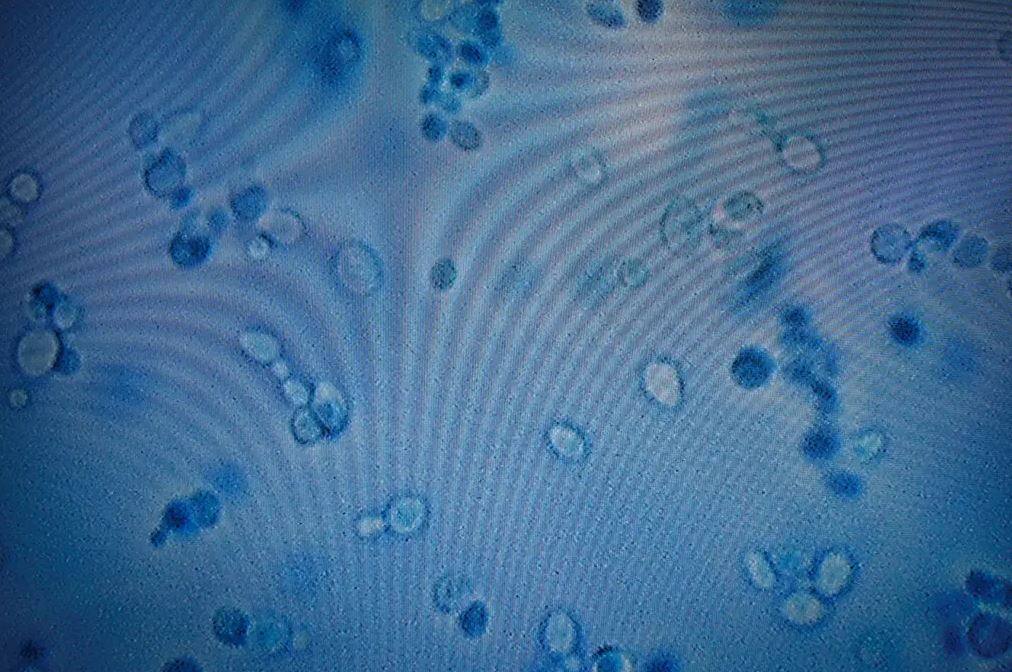
The Centers for Disease Control and Prevention (CDC) said on Monday that a lethal fungus that is regarded as an urgent danger to public health spread at a “alarming pace” during the epidemic.
Candida auris is a particularly deadly fungus because it is resistant to treatment by many of the treatments that are typically used to treat fungal infections. Its primary victims are elderly persons with compromised immune systems. The first case of C. auris was discovered in the United States in 2016, and it was found primarily in the states of New York and Illinois. At the time, public health officials in those states hoped they could stop the spread of the infection by instituting stringent screening and infection control procedures in nursing homes and other long-term care facilities.
Nonetheless, during the course of 2021, state and local health departments throughout the US recorded 1,474 clinical cases, marking an increase of about 200 percent from the roughly 500 cases that were reported in 2019.
According to a study report that was published on Monday in the Annals of Medicine and was produced by researchers at the Centers for Disease Control and Prevention (CDC), the spike marks a “dramatic rise” in both the caseload and transmission of C. auris. The fungus has already been found in 25 of the 50 states, many of which have just a small number of cases, although the states of California, Nevada, Texas, and Florida have the highest numbers.
Caseloads from 2022 were not included in the recently published study. On the other hand, a website maintained by the CDC that monitors the progression of the fungus indicates that 2,377 infections were recorded in 2017, indicating yet another significant rise in the number of cases.
According to the Centers for Disease Control and Prevention (CDC), within three months about half of individuals who get C. auris will pass away. Nevertheless, Dr. Meghan Lyman, a medical officer working in the C.D.C.’s mycotic diseases section, said that the organisation did not have a strong idea of how many fatalities were directly attributable to the fungus. The reason for this is that people who become infected are also dealing with a variety of other health issues. As a result, C. auris has the potential to either be the direct cause of death or something that, in conjunction with other factors contributing to poor health, speeds up the process of dying.
According to the Centers for Disease Control and Prevention (CDC), it is probable that the coronavirus pandemic made the spread of C. auris worse. Because of the focus on Covid-19, screening for C. auris received far less attention than it should have. Moreover, the fungus has a propensity to adhere to nursing gowns, gloves, and other personal protective equipment that, under ideal circumstances, would be changed often but that were reused during the epidemic due of supply shortages. This is another way for the fungus to spread. Moreover, C. auris has the ability to attach itself to ventilators and other types of medical equipment.
C. auris does not pose a significant risk to young healthy individuals since their immune systems are able to fend off the infection; nonetheless, the bacteria may be carried on the skin and on clothes. Individuals who come into contact with it may have normal infection symptoms, including as fever and chills, which may become more severe in the absence of treatment. The fungus most often affects elderly people, and in particular those patients who have frequent or extended trips to medical institutions, where it might be difficult to clean or eliminate the infection completely.
The fact that C. auris may be resistant to antifungal drugs is a significant obstacle in the process of treating the infection. According to the findings of the study article, by the year 2020, 86 percent of the bacterial samples that were evaluated by the Antimicrobial Resistance Laboratory Network of the CDC were resistant to a group of medications called azoles.
The fact that 1.2 percent of C. auris samples were resistant to a first-line therapy class of medications known as echinocandins during that year is more worrisome to the people in charge of public health. In the event that the germ develops to become more resistant to echinocandins, the treatment of C. auris might become highly challenging or perhaps impossible, according to authorities in the health care industry.
Dr. Lyman also said that there is some good news to report. C. auris seems to have been successfully contained inside the health care systems of New York and Illinois, despite the fact that the virus has taken root in other parts of the country, as a result of intensive measures to halt the spread of the germ in those states.