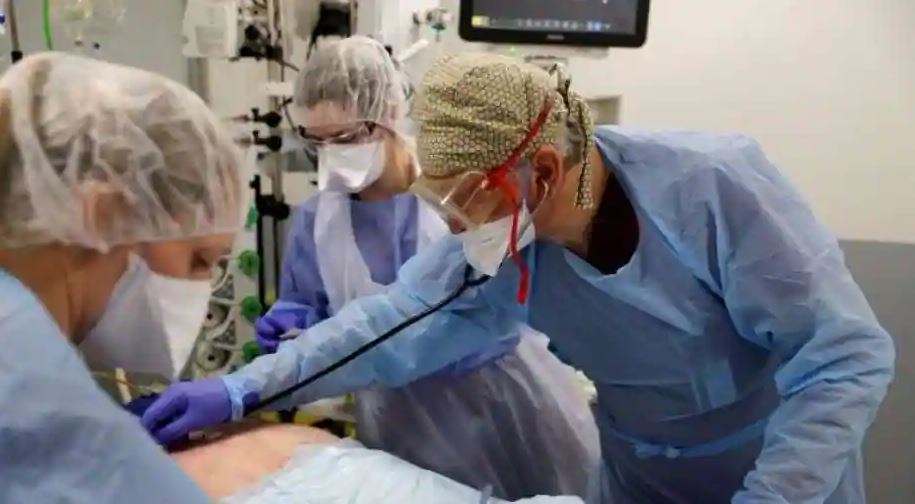
In the critical care unit of Alaska’s biggest hospital, there was one bed that became available.
When the coronavirus outbreak broke out in Anchorage, it was the middle of the night, and the hospital, Providence Alaska Medical Center, had been overwhelmed with patients. Doctors were now faced with a difficult decision: many additional patients in the hospital, the majority of whom were suffering from Covid-19, were waiting in line to occupy the last I.C.U. bed. Someone from one of the state’s remote rural villages, on the other hand, required emergency surgery and had to be airlifted in from another state.
Dr. Steven Floerchinger and his colleagues convened for an excruciating debate about the future of the world. They came to the conclusion that they had a greater chance of rescuing one of the patients in the emergency department.
Since that night, other critical choices have been placed upon Peoples as the state grapples with what is now the world’s leading coronavirus pandemic. Although it’s been nearly two years since the virus first appeared in the United States, some of the scenes here on America’s northern frontier still recall the pandemic’s darkest early days: testing supplies are running low, patients are being treated in hallways, and doctors are restricting the amount of oxygen they can give them. As a result of the overcrowding in the emergency rooms, the governor has requested that hundreds of medical professionals fly in from all across the nation to assist.
Throughout most of the pandemic, Alaska’s natural isolation served to protect the state, with the first few months of the outbreak marked by rigorous testing procedures for visitors from other parts of the world. Many settlements have been closed down. When vaccinations were available, a slew of aircraft, ferries, and sleds were sent to transport doses to remote villages across the world. It has maintained among of the lowest mortality rates in the nation.
However, with some areas of the state wary of vaccines — only about half of the state’s residents have received a full course of vaccination — and Gov. Mike Dunleavy refusing to impose restrictions to contain the virus, the state’s isolation has become a growing liability as the Delta variant sweeps through. The state’s outbreak has persisted despite a national decline in the virus’s prevalence, with new daily cases down by about a third and hospitalizations down by roughly a quarter since September 1.
However, overburdened hospitals in the lower 48 states have had more freedom in transferring patients to nearby cities or other states, while hospitals in the upper 48 states have had less flexibility. In Anchorage, the majority of the assistance comes from Seattle, which is 1,500 miles distant, and hospitals in the Pacific Northwest have been challenged by their own devastating viral epidemic.
Doctors and nurses have begun to speak out at meetings, asking the public to take the virus more seriously, but they have faced resistance on a number of occasions.