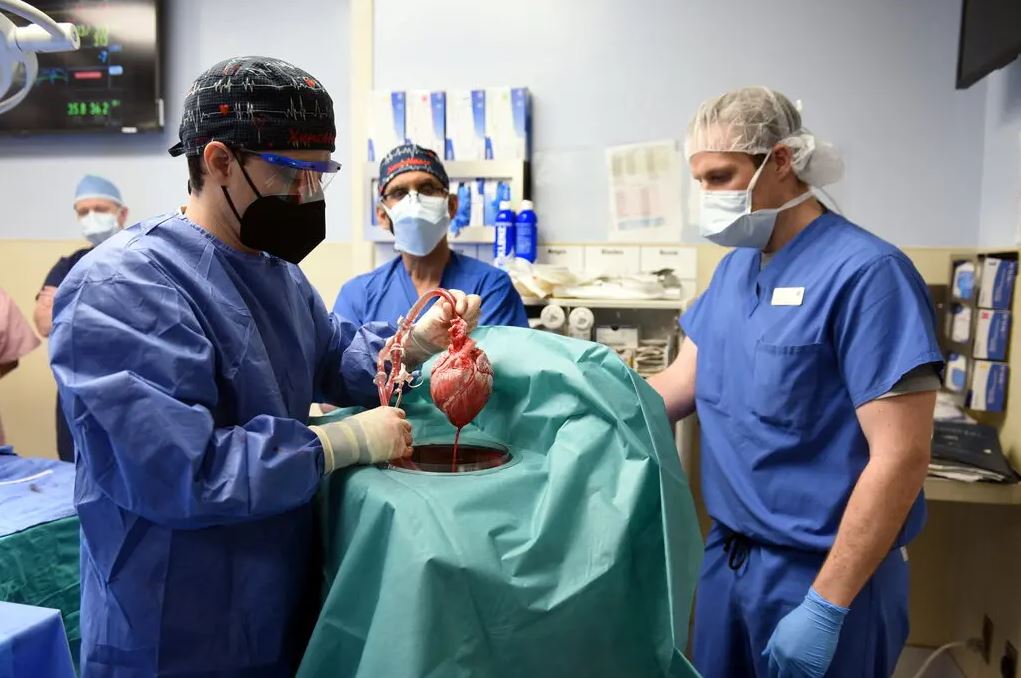
According to the surgeon who conducted the treatment, which was the first of its kind, traces of a virus known to afflict pigs were discovered in the blood of a 57-year-old Maryland man who lived for two months after having his heart transplanted from a genetically altered pig.
The discovery brings to light one of the most compelling arguments against animal-to-human transplantation: the possibility that widespread usage of genetically engineered animal organs might ease the introduction of novel infections into the human population, as has been suggested.
According to Dr. Bartley Griffith of the University of Maryland School of Medicine, the presence of the virus’s DNA in the patient’s bloodstream may have led to his abrupt deterioration more than a month after the transplant. Dr. Griffith performed the transplant.
Dr. Griffith went on to say that there was no sign that the patient had acquired an active viral infection or that his body had rejected the heart during the procedure.
David Bennett Sr., the patient, had been in critical condition before to the operation and had had multiple severe issues as a result of the transplant. He passed away on March 8.
Doctor Griffith’s discoveries concerning viral remnants identified in the patient, presented last month at an American Society of Transplantation conference, were originally published by MIT Technology Review, which is credited with breaking the story.
Dr. Griffith and his colleague, Dr. Muhammad Mohiuddin, the scientific director of the cardiac xenotransplantation programme at the University of Maryland Medical Center, said that they were saddened by Mr. Bennett’s death but that they were not deterred from their goal of using animal organs to save human lives in an interview with The New York Times published on Thursday.
Officials from the company refused to comment on Thursday, and representatives from the Food and Drug Administration, which granted the transplant surgeons an emergency licence for the procedure on New Year’s Eve, said they were unable to quickly reply to inquiries at this time.
Initially, Mr. Bennett’s transplant was judged a complete success. Despite the fact that he did not exhibit indications of rejection, the pig’s heart continued to work for more than a month, marking a significant achievement for transplant patients.
In Mr. Bennett’s case, the presence of swine cytomegalovirus DNA was discovered 20 days after the transplant, but at such a low level that Dr. Griffith speculated that the finding was the result of an unintentional laboratory mistake.
The patient, however, had severe illness around 40 days following the operation, and further testing revealed that his viral DNA levels had increased dramatically, according to Dr. Griffith’s findings.
The heart transplant was one of many innovative transplants performed in recent months that provide hope to the tens of thousands of patients who need new kidneys, hearts, and lungs due to a severe scarcity of given human organs due to a global shortage of donated organs.
Surgeons in New York successfully linked a kidney developed in a genetically engineered pig to a brain-dead patient in October, and discovered that the organ functioned correctly and generated urine after the procedure.
Surgery students at the University of Alabama in Birmingham claimed in January that they successfully transplanted kidneys from a genetically modified pig into the abdomen of a brain-dead man who was 57 years old at the time of the procedure.
However, the danger of unintended effects — notably the introduction of animal infections into the human population — may cause some people to lose interest in the use of genetically engineered organs in the future.
Many experts think that the coronavirus that triggered the worldwide Covid pandemic started with a virus that was transferred from an unnamed animal to humans in China, and that this was the case.
Genetically modified pigs whose organs are to be used for transplantation must be raised in a pathogen-free environment and weaned from their mothers within 48 hours of birth, according to Dr. Jayme Locke, a transplant surgeon and director of the Incompatible Kidney Transplant Program at the University of Alabama at Birmingham. This is necessary to prevent transmission of porcine cytomegalovirus during lactation, according to Dr. Locke.
Such a facility is available at the university, and Dr. Locke said she was still preparing to begin a modest Phase 1 clinical study in which she would transplant kidneys from genetically modified pigs into humans who are nearing the end of their lives with renal disease.