The expanded menu of H.I.V. preventive options for adults and adolescents has received the highest possible recommendation from an important expert group, which means that private insurers will be required to cover the medications.
The verdict specifically targeted H.I.V. prevention medicines licenced for use as pre-exposure prophylaxis (or PrEP), claiming that mandating coverage of these drugs violated the religious freedoms of businesses.
U.S. Preventive Services Task Force granted three licenced drugs for PrEP its highest or “grade A” rating in new guidelines published on Tuesday in JAMA.
The latest decision is an up-to-date support for using a single tablet per day, either Truvada or a generic version, for PrEP. Both cabotegravir (marketed as Apretude) and Descovy (another medication) are now part of the task force.
The new choices may cost more than $20,000 a year, compared to the $1 daily cost of generic Truvada.
There are around 1.2 million people in the United States who have HIV. Now that effective treatments exist, the virus is no longer a death sentence. Although there have been a few miraculous successes in curing HIV, this virus remains incurable, making prevention of new infections a top public health concern.
There were almost 31,000 new cases of HIV in 2020, with nearly 70% of those infections happening in sexually active teenagers and adult males. According to a research conducted in 2018, over 12% of males who have sex only with other men in the United States are HIV positive.
The new recommendations include frequently questioning patients about their experiences with sexual and injectable drug use. The task force concluded that PrEP should be offered to anyone who has a partner who is HIV positive, has recently been diagnosed with a bacterial STD, rarely or never uses condoms, injects drugs, or has a drug-injecting partner who is HIV positive.
However, the Centres for Disease Control and Prevention (C.D.C.) urges doctors to talk about PrEP with all sexually active adults and teenagers and to prescribe it to anybody who asks.
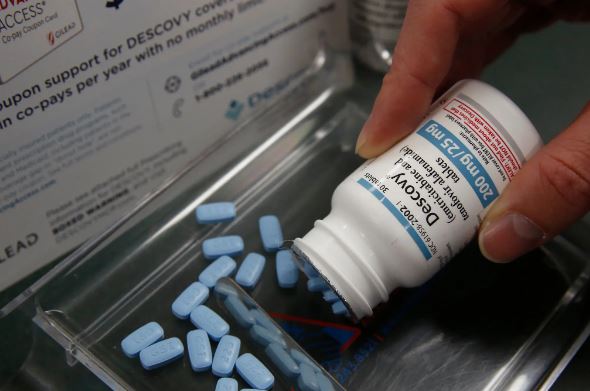
Descovy, another once-daily tablet for H.I.V. prevention, was authorised by the FDA in October 2019 for use by males and transgender women; research on the medicine in cisgender women is just beginning. Descovy may pose less risk of renal damage and bone loss than Truvada does.
The FDA also gave its OK to cabotegravir, a long-acting injection, in December 2021 as a PrEP option. People who are unable or unable to take a daily medication to prevent H.I.V. infection have another option in cabotegravir, which is delivered every two months. Two studies showed that when compared to Truvada and its generic counterparts, the injection was more successful in blocking the spread of H.I.V.
The task group commissioned a systematic assessment of 32 research that demonstrated the advantages of PrEP to update its recommendations for 2019.
In this situation, the task force “acted fairly swiftly to update the recommendation,” as stated by Amy Killelea, a consultant for the advocacy group PrEP4All.
Cisgender males who engage in sexual activity with other men have also been found in many trials to benefit from “on-demand” PrEP using generic Truvada. Two tablets are taken two to twenty-four hours before sexual activity, followed by another pill two days later. The World Health Organisation and the International AIDS Society both agree that this method is productive.
Slow PrEP adoption may be attributed to a variety of factors, including a lack of knowledge and reluctance to take the daily tablets. The proposed regimens, such as providing generic Truvada as the first-line preventative and needing prior permission for the other alternatives, may or may not face resistance from insurance companies.
The risk of contracting any other STD is not reduced by using PrEP. The task force recommended that clinicians frequently test patients for H.I.V. and other sexually transmitted illnesses; educate patients on the need of following their medicines as prescribed; and encourage safe sexual behaviour, including the use of condoms.