Mary Howard, a dishwasher who does not have health insurance, has never received Covid-19 in her life. However, she claims that the coronavirus has led her life to spiral out of control during the last two years.
Friends were killed as a result of it. Even the most routine aspects of her day, such as taking the bus, were fraught with danger. As a result of the pandemic’s impact, the restaurant where she worked had to shut temporarily, and she struggled with depression and high blood pressure, seeking treatment in an emergency hospital since in-person consultations were difficult to come by.
Nashville General Hospital was the place she went for assistance. It has served as the lone public safety-net hospital in a city with a thriving health-care business for more than 130 years, providing treatment to countless impoverished and uninsured individuals during the epidemic and for more than 130 years before that.
After years of funding for uninsured patients and assistance in stabilising hospital budgets during the pandemic, government programmes that paid for Covid treatment are being phased out, posing a new sort of crisis for individuals like Ms. Howard and the doctors who offer them care. Billion dollars in aid not only ensured that uninsured Covid patients would not be burdened with medical bills during the pandemic, but it also provided a lifeline to financially strapped institutions such as Nashville General, which provides extensive uncompensated care for the poor and is in financial trouble.
The infusion of help is coming to an end at a time when Covid-related hospitalizations are down, but at a time when safety-net providers are confronting enormous unmet needs from patients who have delayed treatment for chronic diseases and other health issues much more than normal throughout the epidemic.
Recently, Nashville General has seen an average of just one Covid patient each week, according to the hospital. However, according to the hospital’s physicians and nurses, a broad variety of health conditions that exacerbated during the pandemic are now overwhelming the facility, causing it to close.
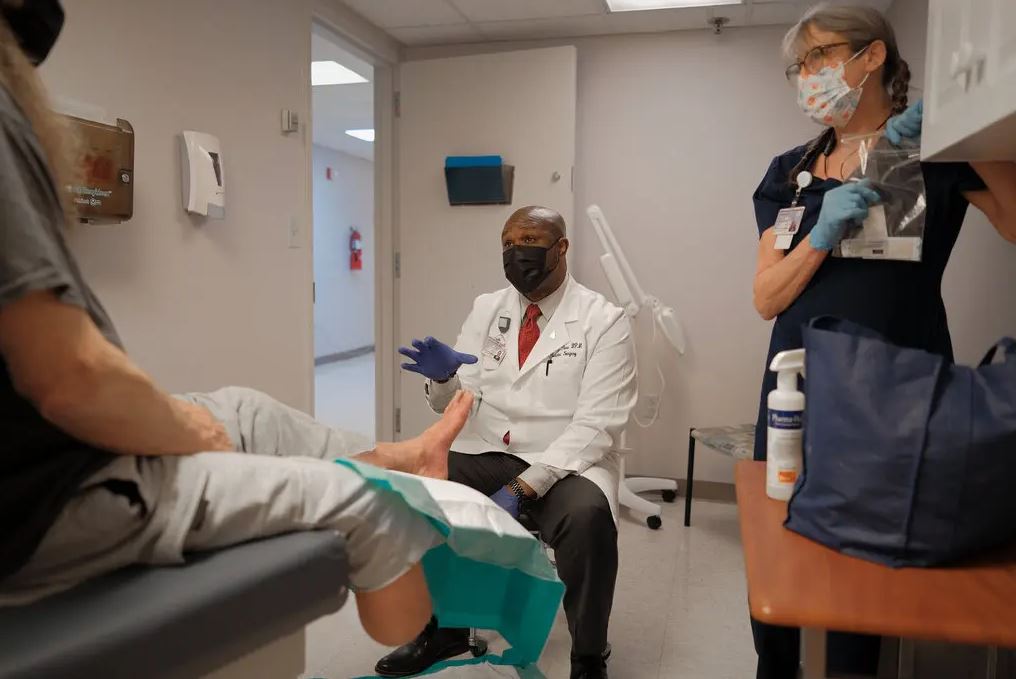
Dr. Andrew Pierre, the hospital’s podiatrist, was preparing to clip a patient’s growing fungal toenails as he explained how the spectrum of uncontrolled issues in his practise had expanded: bunions, flat feet that required reconstructive surgery, and an increase in diabetic sores.
For most of the epidemic, Dr. Eric Neff, an orthopaedic surgeon, stated that patients were scared to go to the hospital, and that they often had difficulty obtaining transportation when they did go. The effects were severe: people delayed seeking treatment for a fractured wrist for six months or neglected a torn rotator cuff for six months, making it more difficult for him to repair their injuries.
Dr. Philip Elizondo, an orthopaedic colleague, said that the hospital was forced to cancel minor procedures due to health issues that grew in severity over the course of the year. One uninsured lady he treated had torn her meniscus, which resulted in her losing her job and her home as a result. Dr. Elizondo said that if the woman had been able to seek treatment promptly, he could have conducted a 20-minute operation, but instead her injuries stayed untreated and worsened, according to him.
Pulmonologist Dr. Richard Fremont said he has treated scores of Covid patients in recent years, but that patients with other health concerns such as persistent asthma were more likely to need oxygen therapy than Covid patients. The fact that uninsured patients cannot get short-term home oxygen treatment means that those who need it are often kept in hospitals for days or even weeks.
Tennessee’s uninsured crisis is particularly acute because the state has one of the highest rates of hospital closures in the country and is one of a dozen states that have chosen not to expand Medicaid to cover more low-income adults as part of the Affordable Care Act’s expansion of coverage for the uninsured. According to the state’s estimates, around 300,000 individuals fall into the so-called coverage gap, which means that, despite having little to no income, they are ineligible for Medicaid or affordable health insurance under the Affordable Care Act.
Health policy expert John Graves of Vanderbilt University School of Medicine claimed that the flood of relief funding during the epidemic had allowed for something close to a “universal coverage system inside a system,” which provided coverage to everyone who received Covid. He claims that hospitals and patients are once again experiencing prepandemic pressures — and that the situation will deteriorate considerably more once the federal government lifts the public health emergency, which has temporarily elevated Medicaid and Medicare payment rates.
In the midst of the epidemic, the federal Provider Relief Fund gave hospitals a lifeline by giving tens of billions of dollars in direct cash, albeit the money was distributed inequitably, according to Jason Buxbaum, a Harvard doctorate student who has written on the programme.
Apart from that, more than $20 billion in payments were made to over 50,000 hospitals, clinics, and other providers for testing and treating the uninsured through the Covid-19 Uninsured Program, with almost $8 million going to Nashville General. An emergency pandemic relief plan that has been blocked in the Senate would almost certainly not refill the fund, leaving providers on the hook and making payouts during future Covid outbreaks doubtful.
Ms. Howard, the dishwasher, expressed her growing dissatisfaction with the process of obtaining and purchasing health insurance. Her illnesses were not getting any better. The day after a recent primary care checkup, she expressed surprise at not being able to come up with the $10 to pay for the visit. “I don’t want to simply be seen or heard,” she said. “I want to be seen and heard.” “It’s difficult when you don’t have any money.”