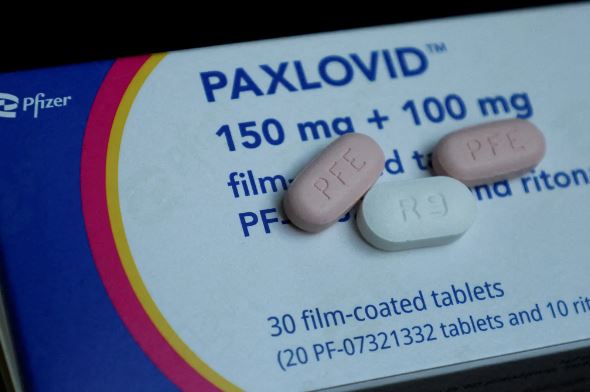In the relentless battle against Covid-19, medical researchers are grappling with a perplexing phenomenon: the underutilization of Paxlovid, a highly effective medication in preventing severe illness and fatalities from the virus. As the nation witnesses a resurgence of Covid, claiming around 1,500 lives each week, scientists are striving to comprehend why Paxlovid, a potent tool in the pandemic arsenal, remains underutilized.
A comprehensive study conducted by the National Institutes of Health (N.I.H.) focused on a million high-risk individuals with Covid, revealing that only approximately 15 percent of those eligible for Paxlovid took advantage of the drug. The implications of this low uptake are stark: the study’s authors estimate that if half of the eligible patients had received Paxlovid during the research period, a staggering 48,000 deaths could have been prevented.
Surprisingly, the reluctance to embrace Paxlovid does not stem from a lack of awareness. The majority of the population is cognizant of the drug’s existence, yet the hesitancy is attributed to concerns voiced by physicians regarding potential drug interactions and individuals wary of a potential rebound case or the drug’s metallic aftertaste.
Analyzing regional disparities provides a glimpse into the puzzle, with higher Paxlovid uptake observed in Democratic strongholds like the Northeast and Pacific Northwest, contrasting with lower utilization in deep red areas such as Florida and Indiana. However, a definitive study elucidating the reasons behind the limited usage of this medication is yet to emerge.
Dr. Josh Fessel, a senior clinical adviser on the N.I.H. team that studied Paxlovid’s utilization, expressed perplexity at the variability and the failure to witness higher adoption across the board. Highlighting the drug’s significant impact, he emphasized that timely Paxlovid administration substantially reduces the likelihood of death or hospitalization.
Covid-related deaths have maintained an elevated trajectory, hovering around 1,200 to 1,300 per week since September, inching up to approximately 1,500 per week in December. Researchers underscore the imperative need for increased uptake of updated Covid vaccines and antiviral treatments to curb this ominous trend.
Dr. Fessel disclosed that throughout the N.I.H. study involving a million high-risk patients eligible for Paxlovid, only around 10 percent opted for the medication, a figure that marginally rose to approximately 15 percent by the study’s conclusion in early 2023. The N.I.H. estimates underscore the potential impact, suggesting that 135,000 hospitalizations and 48,000 deaths could have been averted if half of the eligible patients had availed themselves of the antiviral.
Paxlovid, crafted by Pfizer, constitutes a two-medication treatment designed for consumption within five days of Covid symptom onset to curb viral spread within the body. Approved for adults at high risk of severe Covid, typically those aged 65 and older or individuals with conditions like diabetes and obesity, the drug’s efficacy is undebatable.
Diverse reasons contribute to the reluctance surrounding Paxlovid. Physicians cite reservations about the extensive list of medications incompatible with Paxlovid, including common drugs for blood pressure or clot prevention. Patients express dissatisfaction with the metallic aftertaste, while others dismiss the drug during the initial mild stages of Covid, missing the opportunity to impede early viral growth.
An additional factor influencing Paxlovid usage is its cost. Initially provided at no cost by the federal government following emergency authorization in December 2021 (with full FDA approval in May), the drug is now priced at approximately $1,400 per course by Pfizer. While Medicaid and Medicare patients will continue to receive it for free through 2024, private insurers are expected to cover a portion of the cost, with Pfizer offering co-payment assistance.
Regional disparities in Paxlovid utilization were evident in the N.I.H. study, with rates reaching as high as 50 percent in Utah and Northeast and Northwest regions but plummeting close to zero in Southeastern states and parts of the lower Midwest. The recent transition of Paxlovid distribution to Pfizer adds a layer of complexity, and subsequent studies are needed to assess its impact.
Concerns about Paxlovid rebound, where the drug initially mitigates symptoms but potentially leads to a second stage of illness, may contribute to the hesitancy surrounding the medication. While recent reviews by the Centers for Disease Control and Prevention found “no consistent association” with Paxlovid use and Covid rebound, the misgiving persists.
Denis Nash, a professor of epidemiology at the City University of New York, has delved into Paxlovid usage. His team’s smaller study found uptake at nearly 14 percent, unveiling disparities among different demographics. An ongoing nationally representative survey aims to shed further light on the intricacies of Paxlovid awareness and usage.
Despite the challenges, researchers stress the critical need for increased Paxlovid adoption to mitigate the devastating toll of the ongoing Covid surge. The collective effort to bridge gaps in understanding, dispel misconceptions, and ensure equitable access to effective treatments remains paramount in the ongoing battle against the relentless pandemic.